Corneal Transplant (Partial Penetrating Keratoplasty)
The cornea’s (clear crystal over the iris, or colored part of the eye) main function, in addition to protecting the intraocular contents, is to focus light and therefore it has to be clear and smooth. Generally due to age, disease or trauma, the cornea can become cloudy or irregular and a corneal transplant may become necessary.
The major reasons for a corneal transplant are to:
- Improve vision by replacing the opaque or irregular corneal tissue
- Preserve corneal anatomy and integrity for patients with thinning tissue or reconstruction after corneal perforation
- Remove inflammation of corneal tissue that is unresponsive to antibiotics, etc.
- Improve appearance of corneal scars that cause an opaque or whitish color to the cornea
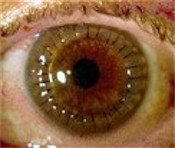 A corneal transplant (corneal grafting or penetrating keratoplasty) is one of the most common and successful of all transplants — about 40,000 are performed each year in the United States. During the procedure a damaged or diseased cornea is replaced with donated corneal tissue which is removed from a recently deceased person and processed by the Georgia Eye Bank.
A corneal transplant (corneal grafting or penetrating keratoplasty) is one of the most common and successful of all transplants — about 40,000 are performed each year in the United States. During the procedure a damaged or diseased cornea is replaced with donated corneal tissue which is removed from a recently deceased person and processed by the Georgia Eye Bank.
The out-patient procedure lasts 30-45 minutes during which the patient is either awake, having received a local anesthetic, or asleep, having received a general anesthetic. It is performed by using a trephine, which looks like a round “cookie-cutter”, to remove only the central portion of a donor cornea. Another trephine is used to remove the central portion of the patient’s cornea. Under a surgical microscope, the donor corneal tissue is placed into the recipient bed and sutured with generally 16-24 microscopic sutures which are finer than a human hair.
After surgery, eye drops are used until the graft heals. Success rates may be as high as 90%, though return of vision can be prolonged, often taking 6 months to 1 year. The sutures are removed painlessly in the office, generally after a year or more.
Descemet’s Stripping (Automated) Endothelial Keratoplasty (DSEK/DSAEK)
The cornea remains clear because the cells on the innermost layer (endothelium) are able to pump fluid out of the cornea, keeping it in a relative dehydrated state. Endothelial cells do not regenerate. We are born with a certain amount and they slowly decrease throughout life. If the endothelial layer is depleted or damaged, the cornea swells and becomes cloudy. Rather than transplanting the full thickness of the central cornea however, we can now, using advanced techniques, transplant just the innermost layers.
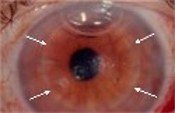 The out-patient procedure lasts 30-45 minutes during which the patient is either awake, having received a local anesthetic, or asleep, having received a general anesthetic. It is performed by using a trephine to remove only the innermost layer of the central portion of a donor cornea obtained from a deceased person and processed by the Georgia Eye Bank. Then using only a very small incision that is either self-healing or may be closed with just a few sutures, the innermost layer of the patient’s cornea is removed and replaced by the donor tissue (as shown by white arrows). An air bubble is placed in the eye to keep the tissue in place. Although only a thin layer of tissue is actually replaced, the graft will help keep the entire cornea clear.
The out-patient procedure lasts 30-45 minutes during which the patient is either awake, having received a local anesthetic, or asleep, having received a general anesthetic. It is performed by using a trephine to remove only the innermost layer of the central portion of a donor cornea obtained from a deceased person and processed by the Georgia Eye Bank. Then using only a very small incision that is either self-healing or may be closed with just a few sutures, the innermost layer of the patient’s cornea is removed and replaced by the donor tissue (as shown by white arrows). An air bubble is placed in the eye to keep the tissue in place. Although only a thin layer of tissue is actually replaced, the graft will help keep the entire cornea clear.
Offering several benefits over traditional methods of corneal transplant, DSEK is less invasive because, instead of removing and replacing the entire thickness of the central cornea, only a small microscopic incision is made. This leaves the eye much stronger and less prone to injury and provides a more rapid rate of visual recovery — 3 to 6 months rather than 1 to 2 years. There are less post-operative visits, fewer sutures to be removed (1-2 versus 16-24) and less chance of rejection and complications.
Dr. Carlin is a highly experienced, board-certified ophthalmologist and Diplomate of the American Board of Ophthalmology with more than five decades of experience in vision care and surgical innovation. A graduate of the University of Illinois College of Medicine, he completed his ophthalmology residency at the University of Michigan before serving in the United States Navy in Key West, Florida. In 1977, he founded CarlinVision and has since built a longstanding reputation for excellence in LASIK, cataract surgery, refractive procedures, and cosmetic eyelid surgery. Throughout his career, Dr. Carlin has completed more than 11,000 procedures and remains at the forefront of advanced laser and refractive technologies. He is a Fellow of the American Academy of Ophthalmology and an active member of multiple leading professional organizations, reflecting his enduring commitment to clinical excellence and patient care.

