Diabetic Retinopathy Review
By Dr. Dimple Modi
What is diabetic retinopathy?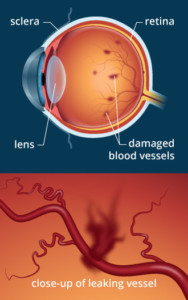
In diabetic retinopathy, the blood vessels of the retina become abnormal, which may cause problems with eyesight. Normally the blood vessels in the retina do not leak. In diabetic retinopathy, the retinal blood vessels develop tiny leaks. Another problem with the retinal blood vessels in diabetes is that they can become obstructed. The areas of the retina in which the blood vessels have become obstructed then foster the growth and increase of abnormal new blood vessels. These changes are caused by chronic high blood glucose levels.
Prevalence of diabetic retinopathy
Greater than 70% of people with diabetes will develop changes to their eyes within 15 years of diagnosis. After 20 years of diabetes, nearly 99% of patients with type 1 Risk factors for developing diabetic retinopathy include:
- How long you have had diabetes
- Poor blood sugar control
- High blood pressure
- High cholesterol
Symptoms of diabetic retinopathy
Diabetic retinopathy may remain asymptomatic in the early stages of the disease. As the disease progresses however, you may experience symptoms such as:
- Blurred vision

- New floaters
- Fluctuating vision
- Distorted vision
- Dark areas or missing vision
- Poor night vision
- Impaired color vision
- Partial or total loss of vision
Prevention and treatment
90% of diabetic eye disease can be prevented simply by regular dilated eye examinations and by tightly controlling your blood sugars. As a diabetic patient, you should at least have annual eye exams by your ophthalmologist, and may even require more frequent exams based on your doctor’s recommendations and the level of diabetic retinopathy in your eyes.
Your doctor may perform some imaging tests to assist with diagnosis of the level of diabetic retinopathy in your eyes which may include photos of the retina. If your central vision is affected by diabetes, your doctor may order a test called Optical Coherence Tomography (OCT). OCT is like an ultrasound which scans the macula, the central most part of the retina, to diagnose swelling from leaky blood vessels.
If you do develop diabetic retinopathy and your doctor recommends treatment, options may include laser or injections.
Laser is a high-energy light that turns to heat when it is focused on the parts of the retina to be treated. Vision may not improve after laser treatment but laser treatment can frequently stop or slow further loss of vision. Your doctor can help you evaluate the benefits and risks of laser and discuss the options with you.
A newer development in treatment option includes an injection into the eye. One factor that causes abnormal blood vessels to grow in the retina in diabetic retinopathy is called vascular endothelial growth factor (VEGF). VEGF can be blocked by a number of medications called anti-VEGF drugs. These medications are directly injected into the eye to target the VEGF and help shrink the blood vessels that are leaking in the back of the eye.
 Another type of medication your doctor may recommend is a steroid injection. Your doctor can best discuss with you your treatment options if needed. The most important and first step is to get your eyes examined to hopefully prevent damage from diabetic retinopathy. The team at CarlinVision is happy to help with all your diabetic eye care needs!
Another type of medication your doctor may recommend is a steroid injection. Your doctor can best discuss with you your treatment options if needed. The most important and first step is to get your eyes examined to hopefully prevent damage from diabetic retinopathy. The team at CarlinVision is happy to help with all your diabetic eye care needs!
Contact Us
Services Contact
Contact Form on the Services page
Dr. Carlin is a highly experienced, board-certified ophthalmologist and Diplomate of the American Board of Ophthalmology with more than five decades of experience in vision care and surgical innovation. A graduate of the University of Illinois College of Medicine, he completed his ophthalmology residency at the University of Michigan before serving in the United States Navy in Key West, Florida. In 1977, he founded CarlinVision and has since built a longstanding reputation for excellence in LASIK, cataract surgery, refractive procedures, and cosmetic eyelid surgery. Throughout his career, Dr. Carlin has completed more than 11,000 procedures and remains at the forefront of advanced laser and refractive technologies. He is a Fellow of the American Academy of Ophthalmology and an active member of multiple leading professional organizations, reflecting his enduring commitment to clinical excellence and patient care.


